Long NHS waiting lists are forcing women in the UK to fundraise to get treated privately for potentially life-threatening gynaecological conditions.
Data from the crowdfunding platform GoFundMe shows that the number of fundraisers mentioning endometriosis, hysterectomy, polycystic ovary syndrome (PCOS) or fibroids has increased by 177 per cent in the past 5 years.
A woman who felt forced to use GoFundMe to help pay for surgery she needed to treat her endometriosis tells Tortoise she is “basically now permanently disabled” because of “gynaecological neglect” by the NHS.
According to GoFundMe, the number of active endometriosis fundraisers in the UK grew by an average of 30 per cent a year between 2018 and 2023.
As of December 2023, there were nearly 600,000 people on NHS gynaecology waiting lists across England, more than 33,000 of those having been waiting over a year.
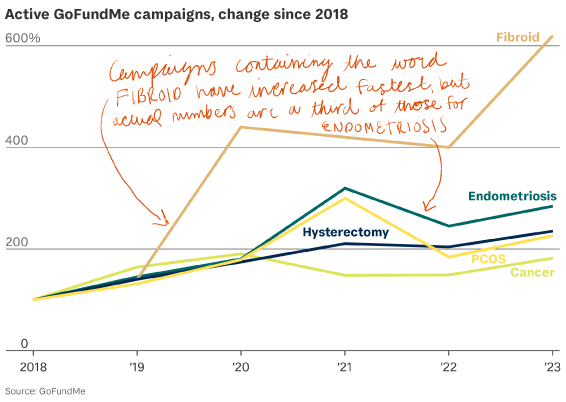
Fundraiser numbers on GoFundMe mentioning hysterectomy, a treatment option for some women with severe endometriosis, have risen on average by 21 per cent year on year since 2018. Tortoise understands fundraiser numbers related to gynaecological conditions are rising faster than overall health-related fundraiser numbers.
The context. Overall NHS waiting list numbers rose to a record 7.75 million last year, while the number of self-paying inpatient and day-case admissions also reached a record of 227,000, according to a Telegraph survey. The number of uninsured patients paying privately for treatment rose from 199,000 in 2019 to 272,000 in 2022.
Endometriosis, which affects around 1.5 million people in the UK, is a condition where cells similar to the ones in the uterus lining are found elsewhere in the body. Symptoms include painful periods and bowel movements, pain during or after sex and infertility.
Currently there is no cure for the condition, but it can be managed with hormone treatments, painkillers and surgery to remove the endometrial lesions – or the uterus itself.
Evelyn Scott, a 36 year-old academic, set up her fundraising page in November 2023 after spending two years waiting for a hysterectomy and seeing “no end in sight”.
Scott’s endometriosis is so severe that she has to take painkillers and laxatives every day, is unable to work or have relationships and has been in and out of emergency hospital care.
She had to contact her local Conservative MP, Leo Docherty, before securing an appointment with an NHS consultant who could perform a hysterectomy.
When she met the consultant in December last year, she was informed she hadn’t been on the NHS hysterectomy waiting list for the past two years – despite having been led to believe otherwise. “So I just had been waiting patiently, my symptoms have been getting worse. I’d been deteriorating – and nothing,” she said.
Scott says a hysterectomy would mean “being able to have a normal life again”. She is currently three-quarters of the way towards her £12,000 target and tells Tortoise she has been contacted by other women trying to raise the money for the operation.
Daneka Etchells, a 29 year-old actor and accessibility consultant, says she has been fighting to get NHS care since she realised something wasn’t right with her periods as a teenager.
Etchells set up a GoFundMe page in November 2023 after being told there was a three to four-year waiting list for the surgery she needed for her severe endometriosis, which would cost more than £11,000 to have done privately.
“I was thinking, at this point, I’m so unwell. I can’t walk unaided for long distances and am frequently having accidents,” she said. “I’m bedridden for four, five, six days of the month. I’m nearly 30 years old and I shouldn’t be thinking about those kinds of things.”
Even when Etchells managed to get an appointment with a private consultant the only reason she could eventually afford the surgery, she says, is that the consultant’s secretary spent two months negotiating down the price at a hospital where she could also get financing.
“These secretaries and these gynaecologists know this is wrong, that they’re making hospitals ‘price match’ for people to get health care,” Etchells says. “They’re on the inside and they work… to ensure people aren’t getting ripped off. That’s the worst thing about it.”
Etchells believes long NHS waiting lists and a poor standard of care for gynaecological conditions are “ruining people’s lives”. She has now had the operation “but I could be infertile now,” she says. “I don’t know. I don’t know if I want to have biological children, but it would have been nice to have a choice.”
Dr Ranee Thakar, President of the Royal College of Obstetricians and Gynaecologists, said:
“The disproportionate growth of gynaecological waiting lists has subjected thousands of women to prolonged suffering grappling with symptoms such as extreme pain, heavy menstrual bleeding and incontinence and we continue to see women’s health deprioritised and overlooked.
“We are asking the NHS to rethink how care is prioritised and consider the wider impacts on the individuals waiting for care. Furthermore, long waits can result in unnecessary emergency admission to hospital, or more complex treatment needs.”
At the beginning of this year the health secretary, Victoria Atkins, said women’s health and maternity care were among her top priorities for 2024. This included better care for menstrual and gynaecological conditions.
A Department of Health and Social Care spokesperson said: “Endometriosis can be a debilitating condition that stops women and girls from living their lives to their fullest potential. Through the Women’s Health Strategy we have set an ambition for all women and girls with severe endometriosis to experience better care with a reduced waiting time for diagnosis.”
An NHS England spokesperson said that the service takes endometriosis “extremely seriously” and that “it is essential that staff support women experiencing cyclical pain as well as the psychological effects associated with their symptoms”.
“The health service is committed to meeting women’s individual healthcare needs and is rolling out dedicated pelvic health clinics – bringing together specialist healthcare staff – to provide further support for women living with endometriosis, as well as supporting all local areas to develop a women’s health hub, to help deliver better menstrual health services and improve women’s health outcomes”, they said.
Further reading: Patients increasingly relying on crowdfunding to pay medical costs in US hospitals.

